Knee Osteoarthritis Treatment in Southampton

Knee Osteoarthritis Treatment in Southampton
That stiffness when you first stand after sitting. The way your knee aches at the end of a long day. The sharp catch when you twist or kneel that makes you second-guess every movement.
If this sounds familiar, you’re not alone.
Knee osteoarthritis is the most common joint condition in the UK, affecting approximately one in five adults over 45 in England. It involves progressive changes to the cartilage, bone, and soft tissues of the knee joint, leading to pain, stiffness, and reduced function. At Southampton Physio on Bedford Place, we use evidence-based physiotherapy to help people with knee osteoarthritis reduce pain, rebuild strength, and return to the activities that matter to them.
Is This What You're Feeling?
You might recognise some of these:
- Morning stiffness that eases after 10–15 minutes of moving around, but returns after you've been sitting for a while
- A deep, achy pain during or after activity — walking, climbing stairs, getting in and out of the car
- Swelling around the knee, especially after a busy day or more activity than usual
- A grinding or clicking sensation when you bend or straighten your knee, sometimes painful, sometimes just unsettling
- Reduced confidence in the knee — you avoid certain movements, choose the other leg first, or plan your day around what your knee can tolerate
These symptoms often build gradually. You might not remember a specific injury. The pain and stiffness accumulate over months or years, shaped by a combination of genetics, previous injuries, activity patterns, and how much load your knee has been asked to manage.
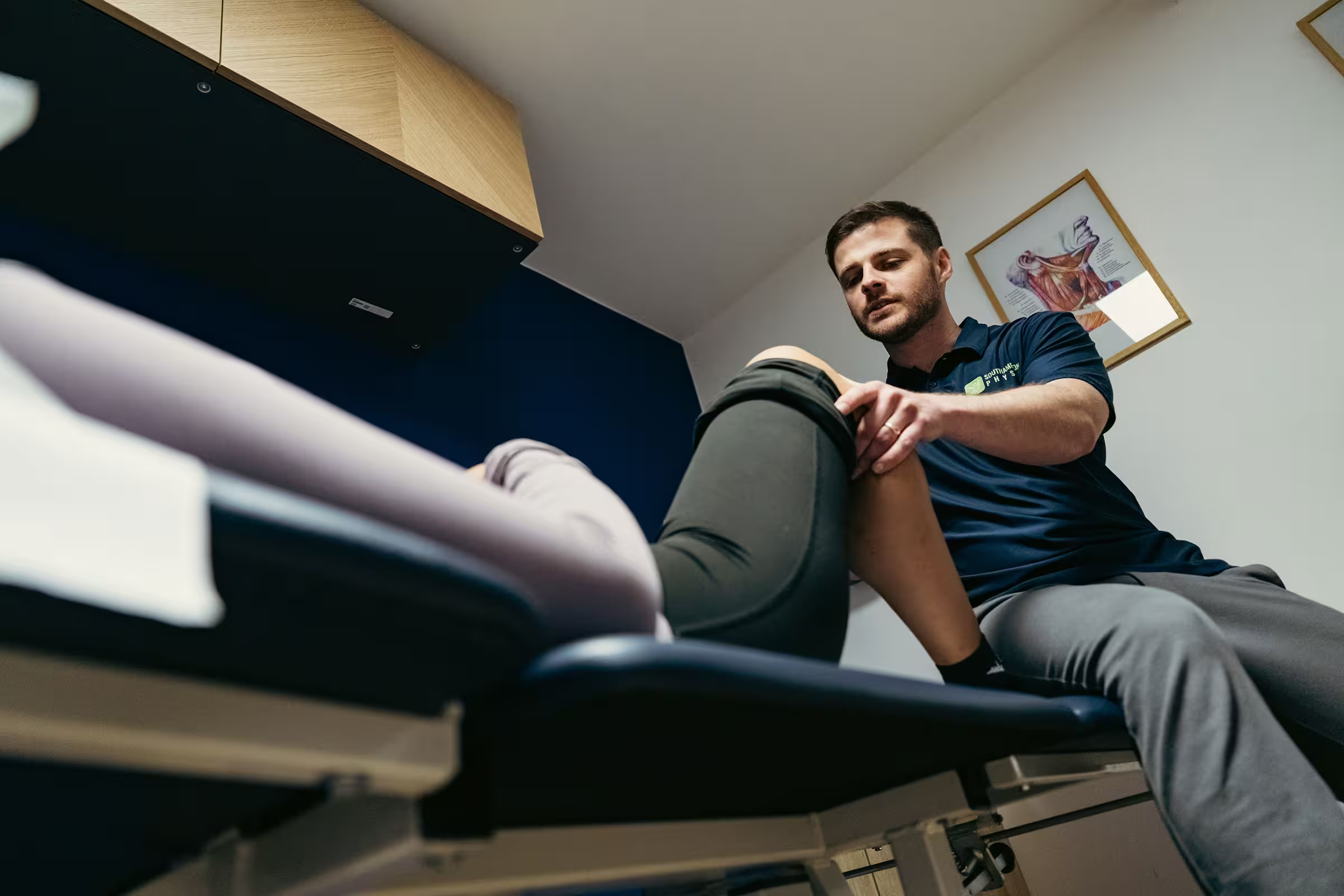
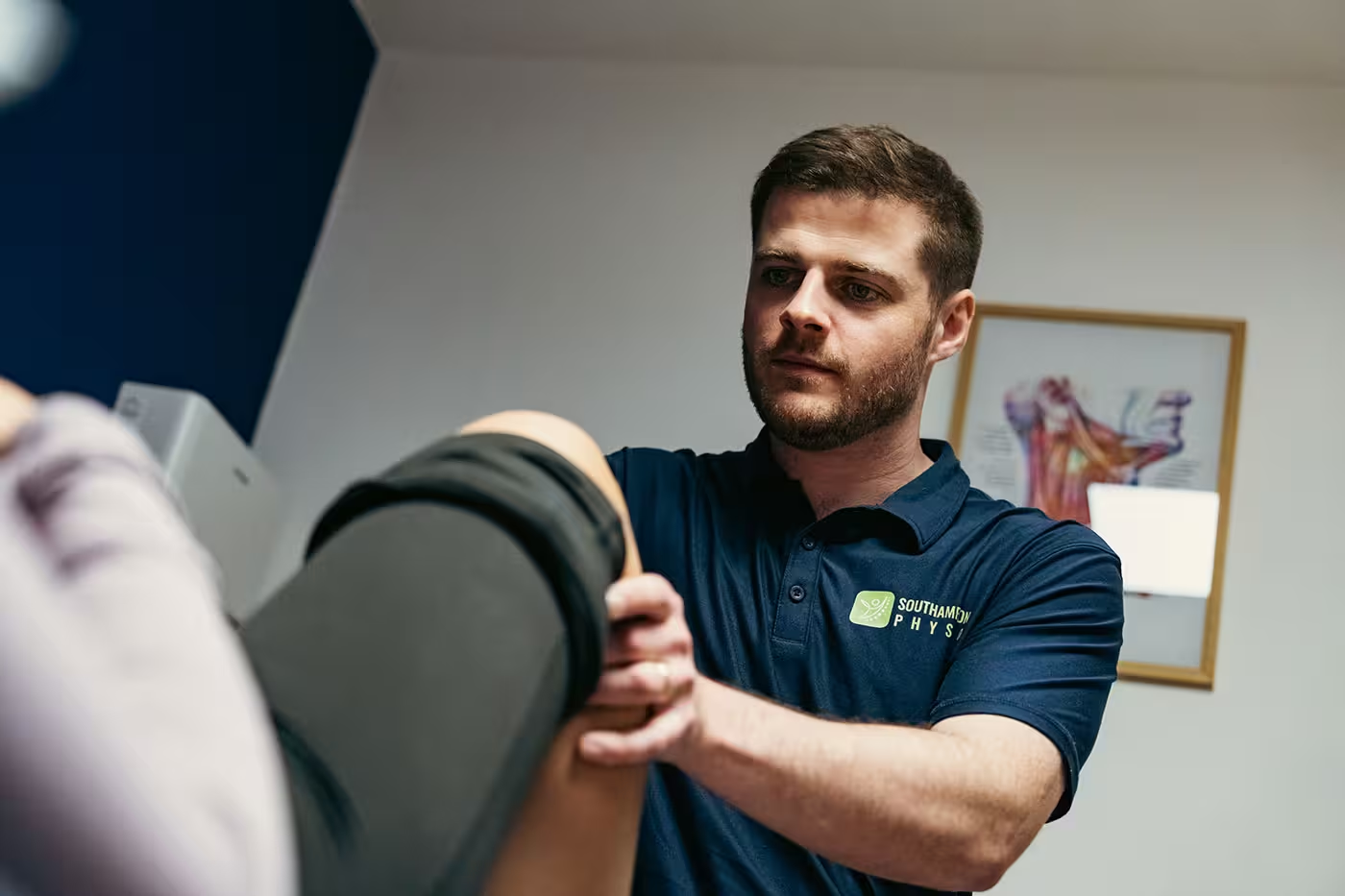
Why Is This Happening?
Knee osteoarthritis develops when the joint’s capacity to tolerate load is exceeded over time. Think of it like a cup filling with water. Stress, lack of movement, previous injuries, and reduced muscle strength all add to the cup. When it overflows, that’s when you feel pain and stiffness.
Cartilage changes are part of the process, but they’re not the whole story. Research published in Osteoarthritis and Cartilage (Swain et al., 2020) shows that the severity of cartilage wear on imaging doesn’t predict how much pain you’ll experience or how well you’ll function. Many people with significant cartilage changes on scans have little or no pain, while others with minor changes report substantial symptoms.
What matters more is the strength and capacity of the muscles around the knee, particularly the quadriceps and hip muscles. When these muscles are weak or not working efficiently, the knee joint absorbs more force with every step. Over time, this overload contributes to inflammation, pain, and further loss of confidence in the joint.
Other factors that often play a role include:
- Obesity — the largest modifiable risk factor for knee osteoarthritis progression. Excess adipose tissue produces pro-inflammatory cytokines, creating a systemic inflammatory environment that contributes to cartilage breakdown and joint deterioration.
- Previous knee injury — a torn meniscus, ligament injury, or fracture can alter the way forces distribute across the joint.
- Occupational exposure — jobs that involve repetitive kneeling, squatting, or heavy lifting increase risk (odds ratio 1.9, 95% CI: 1.3–2.8).
- Inactivity — prolonged lack of movement weakens the muscles that protect the knee and reduces the joint's tolerance for load.
- Malalignment — varus (bow-legged) or valgus (knock-kneed) patterns can concentrate force on one side of the joint.
The good news is that pain and function can improve significantly with the right approach, even when structural changes are present. The 2024 Cochrane review of exercise for knee osteoarthritis, which included 139 trials and 12,468 participants, found that exercise therapy produces moderate effects on pain and function immediately after treatment, with small effects sustained at two to five months (Lawford et al., 2024).
How Southampton Physio Treats Knee Osteoarthritis
Current evidence and clinical guidelines, including NICE (2022) and the updated EULAR recommendations (Moseng et al., 2024), are clear: exercise therapy, patient education, and weight management (where relevant) are the foundation of treatment for knee osteoarthritis. Manual therapy can help in the short term, but it’s an adjunct — not a standalone fix.
Your First Assessment
Outcome: A clear diagnosis and a treatment plan tailored to your knee, your goals, and your life.
Your first session lasts around 45 minutes. We’ll take a detailed history: when the pain started, what makes it better or worse, what you’ve tried already, and what you’re hoping to get back to. We’ll assess your knee’s range of motion, strength, and movement patterns, and we’ll look at how your hip and ankle contribute to the overall picture.
If you’ve had scans, bring them — they’re helpful context. But we won’t base your prognosis on imaging alone. What matters more is how you move, how strong you are, and how confident you feel in the joint.
By the end of the session, you’ll understand what’s happening, why it’s happening, and what we can do about it.
Hands-On Treatment
Outcome: Short-term symptom relief and preparation for exercise.
Manual therapy — soft tissue work, joint mobilisation, and hands-on techniques — can reduce pain and improve movement in the short term. Research co-authored by Ian Greaves, published in the International Journal of Osteopathic Medicine (2024), explores how manual approaches can support recovery when integrated with active rehabilitation.
NICE guidelines recommend manual therapy only as an adjunct to exercise, not as a standalone treatment. We use it to settle irritable symptoms, improve joint mobility, and help you feel more comfortable moving. But the lasting benefit comes from what you do next: building strength and capacity.
Building Long-Term Strength
Outcome: Stronger, more resilient muscles that protect your knee and reduce pain over time.
This is where the real work happens. Progressive, individualised exercise is the most effective treatment for knee osteoarthritis. EULAR guidelines give it the highest strength of recommendation (LoE 1a, SoR A, Level of Agreement 9.5/10).
We design a programme that combines:
- Quadriceps strengthening — the muscles at the front of your thigh absorb force and protect the knee joint. Stronger quads reduce pain and improve function.
- Hip strengthening — weak hip muscles (glutes and hip abductors) can alter knee alignment and increase joint stress. Addressing this improves movement patterns.
- Aerobic exercise — walking, cycling, or swimming builds general fitness and supports long-term joint health.
- Neuromuscular training — balance and coordination exercises improve confidence and reduce the risk of falls or sudden twists.
Your programme starts at a level you can manage and progresses gradually. Joints need progressive load to strengthen. Too much too soon overloads them; too little and they weaken. We supervise your exercises closely in the early stages, then support you to continue independently as confidence and capacity build.
For some people, especially those who’ve tried multiple treatments without lasting results, we offer a more comprehensive pathway that integrates our full team over 12–16 weeks. This is designed for persistent or complex issues that need a deeper root-cause approach.


What You Can Start Doing Today
While you’re waiting for your first session, here are three things you can do now:
- Keep moving. Inactivity weakens the muscles around your knee and reduces the joint’s tolerance for load. Walking, cycling, or swimming — even in short bouts — is better than rest. If your knee is irritable, reduce intensity or duration, but don’t stop completely.
- Manage your weight if you’re overweight. NICE and EULAR guidelines recommend a 5–10% body weight reduction for people with knee osteoarthritis who are overweight or obese. Even modest weight loss reduces systemic inflammation and can significantly improve symptoms.
- Use heat or cold for symptom relief. A hot water bottle before activity can ease stiffness. Ice after activity can settle inflammation. Both are safe, low-cost adjuncts to exercise.
When Should You Be Concerned?
Most knee pain from osteoarthritis improves with physiotherapy and exercise. But if you notice any of these, contact your GP urgently:
- Sudden onset of severe pain, swelling, and fever — this could indicate septic arthritis, a medical emergency. Septic arthritis must be considered and promptly diagnosed in any patient presenting with acute atraumatic joint pain, swelling, and fever (AAFP, 2021). The knee is the most common joint involved.
- Unrelenting night pain unrelated to activity, especially with unexplained weight loss or a history of cancer — this may indicate a more serious underlying condition.
- Bilateral, symmetrical joint swelling with morning stiffness lasting more than 30 minutes — this may suggest inflammatory arthritis, which requires different management.
If you’re unsure, book an assessment. We’ll identify red flags and refer appropriately if needed.


What to Expect: Your Recovery Timeline
Knee osteoarthritis is a long-term condition with no cure. The goal of treatment is symptom control, improved function, and slowing progression. Most people see meaningful improvement within 6–12 weeks of starting a structured exercise programme.
The 2024 Cochrane review found that exercise produces moderate effects on pain and function immediately after treatment, with small effects sustained at two to five months (Lawford et al., 2024). Longer-term benefits depend on continued adherence. Booster sessions — periodic return visits to refine your programme and address setbacks — show small to moderate effects for improving mid-term to long-term exercise adherence.
Factors associated with better outcomes:
- Higher baseline function and strength
- Lower BMI or successful weight loss
- Good exercise adherence and self-efficacy
- Absence of significant comorbidities or widespread pain
Factors associated with slower progress:
- Obesity
- Severe structural changes (Kellgren-Lawrence grade 3–4 on imaging)
- Bilateral involvement
- Psychological comorbidity (depression, anxiety, catastrophising)
- Varus or valgus malalignment
Even with these challenges, most people improve with the right support.
Why Choose Southampton Physio for Knee Osteoarthritis?
We’re a small, experienced team based on Bedford Place in central Southampton (SO15 2DG). We’ve worked with hundreds of people with knee osteoarthritis — from office workers who want to walk without pain to runners rebuilding after years of setbacks.
Our approach is evidence-based, not sales-driven. We don’t offer treatments that NICE guidelines recommend against (acupuncture, glucosamine, hyaluronic acid injections). We don’t promise cures. We focus on what works: exercise, education, and long-term capacity building.
Research co-authored by Ian Greaves and published in the International Journal of Osteopathic Medicine (2024) informs our manual therapy approach. We integrate osteopathy, physiotherapy, sports therapy, and clinical personal training under one roof, so you get continuity of care without being referred elsewhere.
[TESTIMONIAL: “Well what can I say I’m in so much of a better place than what I was nearly a year ago. I’ve suffered from bad knees for years, and bit the bullet and decided enough was enough. From the moment I had an initial phone call to appointments every 2 weeks its been well worth it. Ewan is great he is very easy to talk to, he listens to what you are saying. He explains things very well. Ewan and I have had lots of laughs, and I’ve cried many times when I’ve had setbacks. But he picks you up and explains that sometimes setbacks are good. I’ve now finished my journey my knees are in so much of a better place, I would highly recommend them especially Ewan.” — Sally Cardigan]


Frequently Asked Questions About Knee Osteoarthritis in Southampton
Can physiotherapy help knee arthritis?
Yes. Current evidence shows that exercise therapy, supervised by a physiotherapist, produces moderate effects on pain and function for people with knee osteoarthritis. A 2024 Cochrane review of 139 trials found that benefits are sustained at two to five months, with longer-term outcomes dependent on continued exercise adherence. NICE and EULAR guidelines both recommend physiotherapy-led exercise as a first-line treatment.
What is the best exercise for osteoarthritis?
A combination of strengthening exercises (particularly for the quadriceps and hip muscles), aerobic activities (walking, cycling, swimming), and neuromuscular training (balance and coordination work) is most effective. The best exercise is one you can do consistently, tailored to your current capacity and progressed gradually over time.
How long does physiotherapy take to help knee arthritis?
Most people notice improvements in pain and function within 6–12 weeks of starting a structured exercise programme. Immediate post-treatment effects are moderate, with smaller sustained effects at two to five months. Long-term benefit depends on ongoing adherence and periodic booster sessions.
Is it safe to exercise with knee osteoarthritis?
Yes. Exercise is safe and recommended. Some discomfort during or after exercise is normal, especially in the early stages. Pain that settles within 24 hours and doesn’t progressively worsen is acceptable. Your physiotherapist will help you find the right balance between challenge and tolerance.
What should I avoid with knee osteoarthritis?
Avoid prolonged inactivity — rest weakens the muscles that protect your knee. NICE guidelines recommend against acupuncture, glucosamine, and chondroitin supplements due to lack of evidence. Hyaluronic acid injections are also not recommended, as they show no clinically meaningful benefit and carry a higher risk of serious adverse events compared to placebo.
When should I see a physiotherapist for knee pain?
If knee pain is affecting your daily life, limiting your activity, or causing you to avoid movements you used to do comfortably, it’s time to see a physiotherapist. Early intervention — before pain becomes persistent and muscles weaken significantly — tends to produce faster and better outcomes.
Do I need a scan for knee osteoarthritis?
Not usually. Diagnosis is primarily clinical, based on your symptoms, history, and physical examination. Scans (X-rays or MRI) can confirm structural changes, but they don’t predict how much pain you’ll have or how well you’ll respond to treatment. Many people with significant changes on imaging have little pain, and vice versa. We’ll refer for imaging if there’s uncertainty about the diagnosis or if surgery is being considered.
What causes an osteoarthritis flare?
Flare-ups — periods of increased pain and stiffness — can be triggered by a sudden increase in activity, prolonged inactivity, stress, poor sleep, or changes in weight. Sometimes there’s no obvious trigger. Flare-ups are a normal part of managing a long-term condition. They don’t mean you’ve caused permanent damage. Return to the basics: gentle movement, load management, and symptom-settling strategies like heat or ice.
Will I need a knee replacement?
Most people with knee osteoarthritis do not need surgery. Joint replacement is considered when symptoms substantially affect quality of life and haven’t responded to non-surgical treatment, including physiotherapy, weight management, and appropriate pharmacological management. Almost all (98%) of knee replacements in the UK are due to osteoarthritis, but this represents a small proportion of people living with the condition.
Does walking help with knee arthritis?
Yes. Walking is a safe, low-impact aerobic activity that helps maintain joint health, builds general fitness, and strengthens the muscles around your knee. Start at a level you can tolerate and build gradually. If walking is painful, reduce the distance or intensity, but avoid stopping completely unless advised otherwise.
Booking
Ready to Get Moving Again?
Knee osteoarthritis doesn’t have to stop you from doing the things you enjoy. With the right support, most people see significant improvements in pain and function, even when structural changes are present.
We’ll assess your knee, explain what’s happening, and build a programme that works for your life. No false promises. No passive treatments. Just clear, evidence-based care that helps you rebuild strength and confidence.
Call us on 023 8110 2077 or book online today.
Written by Ian Greaves, MOst, Registered Osteopath (GOsC 11228), iO 106967